Survivorship Resources
During their active treatment period, breast cancer patients have many questions. Once treatment is finished, there are often a whole new set of concerns. Patients vary in their information needs and their timing, and during this time patients may not be seeing their treatment team as frequently in person, as they were during active treatment. Although patients are provided with information on diet and exercise at the time of diagnosis, this is often understandably put to one side during treatment. As such it can be helpful for all these resources to be available in one place for patients to be able to access at time that is appropriate for them.
Survivorship Challenges
Cancer is often described as a journey that starts at diagnosis. During treatment, some people feel that their life is on hold. After treatment ends, it may be hard to know how to resume normal activities. Survivors may expect life to return to what it was like before the cancer diagnosis. For many people, though, it isn’t that simple. The reality is often more emotionally and physically complex. Some cancer survivors find they can’t or don’t want to go back to how life was before their treatment. Many survivors say that cancer changes them. After treatment, they may feel different, even though they look the same. With time, survivors often find a new way of living. Many call this a ‘new normal’. It may take months or years to find a ‘new normal’.
The concept of cancer survivorship—moving past a diagnosis of cancer with all that means and back into a life with your “new normal—is fairly new. Even though treatment is finished, many survivors feel a letdown. It is frightening to finish treatment! While you are going through surgery, chemotherapy, or radiation therapy, you are likely supported and surrounded by loved ones not to speak of being in close touch with your medical providers. When that ends you can feel a lot of fear and even a sense of loss.
For most people, their bodies are not the same. Cancer fatigue may continue for years, and studies tell us that a significant number of people are left with chronic medical or emotional concerns following treatment.
![]() Managing the late effects of breast cancer treatment
Managing the late effects of breast cancer treatment
Even with these advances, many people feel abandoned when active treatment is through. It’s like there’s an unspoken word which states, “You survived, be happy, now go and have a good life.” Not only do many people have no idea what that is supposed to look like, but they are left wondering how they are going to cope with the residual effects of the treatment.
For this reason, cancer survivorship is the newest frontier in managing cancer following treatment. Cancer rehabilitation is now making a difference for many people. If you have finished treatment – or will in the near future – talk to your doctor about the possibility of rehabilitation so that your “new normal” can be a better new normal.
Breast Cancer Prehabilitation / Rehabilitation Programmes
During the cancer journey, two types of assessment may be undertaken:
(1) Prehabilitation “prehab” Assessment Pre-treatment
(2) Rehabilitation “rehab” Assessment early Post-Treatment
Cancer Prehabilitation has been defined as “a process on the cancer continuum of care that occurs between the time of cancer diagnosis and the beginning of acute treatment and includes physical and psychological assessments that establish a baseline functional level, identify impairments, and provide interventions that promote physical and psychological health to reduce the incidence and/or severity of future impairments.”
In breast cancer patients in whom surgery is the initial treatment modality, surgery usually takes place very soon after the time of diagnosis, and as such, there is little time for “prehab” to take place. In the growing number of women however who are treated with initial drug therapy prior to their surgery, ie neoadjuvant chemotherapy, surgery does not take place for at least 3-6 months, and these women should all be ideally referred for participation in an oncology prehabilitation programme.
The goal of prehabilitation is to prevent or reduce the severity of anticipated treatment-related physical impairments and psychological distress that may cause significant disability. Cancer prehabilitation is the first part of the process of rehabilitation. The evidence suggests that it should occur between the time of diagnosis and the start of acute oncology treatment, and that the intervention of prehabilitation could help the patients maintain a better physical function status compared to those without prehabilitation intervention before surgery. Furthermore, an important point is that the interventions for prehabilitation before active treatment are not only limited to use before cancer treatment begins, but may also continue throughout survivorship.
It has been reported that prehabilitation programs could improve physical and psychological health outcomes and reduce surgical complication, treatment–related morbidity, hospital lengths of stay, hospital readmissions, and overall health care costs.
All breast cancer patients undergoing their treatment at St Vincent’s Private East Melbourne are encouraged to participate in the SVPHEM Outpatient Oncology Prehabilitation and Rehabilitation Programmes. At our East Melbourne Day Therapies Unit we run programmes designed to provide individualised exercise therapy and practical ways to help improve and manage your condition and maximise the potential for recovery.
What we offer:
- Comprehensive physiotherapy assessment including individualised exercise prescription for before, during or after treatment.
- Lymphoedema screening.
- Dietitian services to manage nutritional needs before, during and after treatment.
- Occupational therapy to assist with increasing independence and returning to everyday activities at home and in the community, including a focus on fatigue management and return to work strategies.
- Psychology education and strategies to help you cope with cancer including stress management and how to use relaxation and positivity to improve wellbeing.
- Liaison and consultation with external supports for ongoing care and rehabilitation.
- Group programmes which include individualised exercise for strengthening and fitness and education sessions on common cancer related concerns, including physical activity, nutrition, fatigue management, emotional wellbeing and sleep.
![]() St Vincent’s Private Hospital East Melbourne Oncology Day Therapy Rehabilitation
St Vincent’s Private Hospital East Melbourne Oncology Day Therapy Rehabilitation
General References
Survivorship Exercise in Cancer Care Clinical research has established exercise as a safe and effective intervention to counteract many of the adverse physical and psychological effects of cancer and its treatment. To date, the strongest evidence exists for improving physical function (including aerobic fitness, muscular strength and functional ability), attenuating cancer-related fatigue, alleviating psychological distress and improving quality of life across multiple general health and cancer- specific domains. Emerging evidence highlights that regular exercise before, during and following cancer treatment decreases the severity of other adverse side effects and is associated with reduced risk of developing new cancers and comorbid conditions such as cardiovascular disease, diabetes and osteoporosis. Moreover, epidemiological research suggests that being physically active provides a protective effect against cancer recurrence, cancer-specific mortality and all-cause mortality. The convincing body of epidemiological and clinical trial evidence on the benefits of exercise has led to the endorsement of exercise guidelines for people with cancer by major organisations internationally. These guidelines largely mirror guidelines for the general population. Despite this advice being widely disseminated by government and non-government cancer organisations, the majority of Australians with cancer do not meet these recommended targets. Reports indicate that 60-70% of people with cancer do not meet aerobic exercise guidelines and it is estimated that 80-90% do not meet resistance exercise guidelines. Thus, although many people with cancer have indicated a desire to participate in appropriately designed and supervised exercise programs, only a minority are engaging in sufficient levels of exercise. The Clinical Oncology Society of Australia (COSA) position statement on exercise in cancer care outlines the society’s position on exercise recommendations: EX-MED Cancer is a best-practice exercise medicine program providing individualised exercise prescriptions to people with cancer. “If the effects of exercise could be encapsulated in a pill it would be prescribed to every person with cancer. Even if this pill had just a fraction of the positive health benefits exercise provides it would be viewed as a miracle drug in the fight against cancer.” EX-MED Cancer incorporates a coordinated pathway of care between cancer specialists, general practitioners and exercise physiologists within the treatment plan of people with cancer. EX-MED Cancer is a 4-month exercise medicine program designed for people with cancer based on the latest scientific advances. Patients receive an individually prescribed specifically tailored exercise medicine program. You and will be exercising with a small group of other cancer patients at a fitness centre close to your home or work, supervised by qualified exercise physiologists who specialise in exercise for people with cancer. EX-MED Cancer is an Australian Charities and Not-for-profit Commission registered not-for-profit organisation. See: https://www.exmedcancer.org.au Exercise and Physical Activity in Breast Cancer Survivors Diet and Nutrition Following Breast Cancer See Body Weight and Breast Cancer Breast Cancer and Bone Health Breast Cancer and Sexuality Breast Cancer and Mental Health Lymphoedema Managing Menopausal Symptoms After Breast Cancer Travel Insurance You will need the Adobe Reader to view and print these documents.![]() Lifestyle modifications for patients with breast cancer to improve prognosis and optimize overall health
Lifestyle modifications for patients with breast cancer to improve prognosis and optimize overall health
![]() American Society of Clinical Oncology Position Statement on Obesity and Cancer
American Society of Clinical Oncology Position Statement on Obesity and Cancer![]() Survivorship care after breast cancer
Survivorship care after breast cancer![]() Facing Forward -Life After Cancer Treatment
Facing Forward -Life After Cancer Treatment![]() What’s Next? -A Young Woman’s Post-Treatment Navigator
What’s Next? -A Young Woman’s Post-Treatment Navigator


![]() Clinical Oncology Society of Australia position statement on exercise in cancer care
Clinical Oncology Society of Australia position statement on exercise in cancer care ![]() The Exercise and Sports Science Australia position statement: Exercise medicine in cancer management
The Exercise and Sports Science Australia position statement: Exercise medicine in cancer management ![]() Exercise Is Medicine in Oncology: Engaging Clinicians to Help Patients Move Through Cancer
Exercise Is Medicine in Oncology: Engaging Clinicians to Help Patients Move Through Cancer 
![]() EX-MED Cancer for Health Professionals
EX-MED Cancer for Health Professionals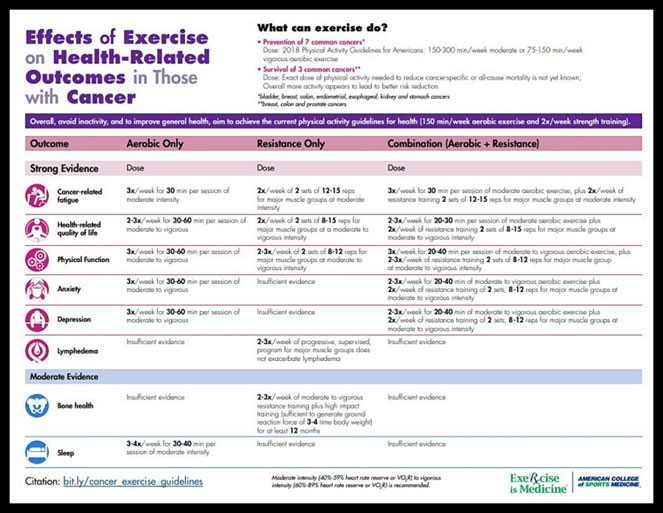
![]() Exercise for People Living with Cancer
Exercise for People Living with Cancer![]() Diet, Nutrition, Physical Activity and Breast Cancer Survivors
Diet, Nutrition, Physical Activity and Breast Cancer Survivors![]() Guidelines for implementing exercise programs for cancer patients
Guidelines for implementing exercise programs for cancer patients![]() Nutrition and Lifestyle after Breast Cancer
Nutrition and Lifestyle after Breast Cancer![]() Healthy Eating and Breast Cancer
Healthy Eating and Breast Cancer![]() Managing Your Weight After A Cancer Diagnosis
Managing Your Weight After A Cancer Diagnosis![]() Managing weight gain after cancer treatment
Managing weight gain after cancer treatment ![]() American Society of Clinical Oncology Position Statement on Obesity and Cancer
American Society of Clinical Oncology Position Statement on Obesity and Cancer![]() Diet, Nutrition, Physical Activity and Breast Cancer Survivors
Diet, Nutrition, Physical Activity and Breast Cancer Survivors![]() Osteoporosis and breast cancer treatment
Osteoporosis and breast cancer treatment![]() What you need to know about Osteoporosis
What you need to know about Osteoporosis![]() Breast Cancer and Sexual Wellbeing
Breast Cancer and Sexual Wellbeing![]() Sexuality, Intimacy and Cancer
Sexuality, Intimacy and Cancer![]() Anxiety, Depression and Breast Cancer
Anxiety, Depression and Breast Cancer![]() GP Mental Health Treatment Plan
GP Mental Health Treatment Plan![]() Lymphoedema-What you need to know
Lymphoedema-What you need to know![]() Reducing the Risk of Lymphoedema
Reducing the Risk of Lymphoedema![]() Understanding Lymphoedema -A guide for people affected by cancer
Understanding Lymphoedema -A guide for people affected by cancer![]() The Diagnosis and Treatment of Lymphedema
The Diagnosis and Treatment of Lymphedema![]() Lymphedema Risk Reduction Practices
Lymphedema Risk Reduction Practices![]() Screening and Early Detection of Breast Cancer- Related Lymphedema: The Imperative
Screening and Early Detection of Breast Cancer- Related Lymphedema: The Imperative![]() Managing Menopausal Symptoms After Breast Cancer
Managing Menopausal Symptoms After Breast Cancer![]() Menopausal Symptoms and Breast Cancer
Menopausal Symptoms and Breast Cancer![]() Treating Hot Flushes: An Alternative to Menopausal Hormone Therapy
Treating Hot Flushes: An Alternative to Menopausal Hormone Therapy![]() Managing Your Menopause After Breast Cancer
Managing Your Menopause After Breast Cancer![]() Breast Cancer and Early Menopause
Breast Cancer and Early Menopause![]() Early Menopause due to Chemotherapy and Radiotherapy
Early Menopause due to Chemotherapy and Radiotherapy ![]() Lifestyle and behavioural modifications for menopausal symptoms
Lifestyle and behavioural modifications for menopausal symptoms![]() Non-hormonal Treatments for Menopausal Symptoms
Non-hormonal Treatments for Menopausal Symptoms![]() Understanding Menopause-Advice for Women who are receiving hormonal therapy for breast cancer
Understanding Menopause-Advice for Women who are receiving hormonal therapy for breast cancer![]() Hot Flushes- Advice for Women who are receiving hormonal therapy for breast cancer
Hot Flushes- Advice for Women who are receiving hormonal therapy for breast cancer![]() Vaginal Health After Breast Cancer
Vaginal Health After Breast Cancer![]() Management of Menopause in the Breast Cancer Patient
Management of Menopause in the Breast Cancer Patient![]() Travel Insurance after Early Breast Cancer
Travel Insurance after Early Breast Cancer
![]()
















