Microcalcification/Hookwire Localisation
What are breast calcifications?
Breast calcifications are tiny calcium deposits that sometimes form in the breast. They are common and found on about half of all mammograms. Calcifications usually develop naturally as the breast tissue ages. They are not caused by calcium in the diet and there is no known relationship between the amount of calcium in a woman’s diet and breast calcifications. Sometimes they form because of other changes in the breast – for example a benign breast condition such as a fibroadenoma or cyst. Calcifications can also form if you’ve had an infection in, or injury to the breast, or if you’ve had stitches or a breast implant.
Calcifications may also develop in the blood vessels of the breast. These vascular calcifications are rare in younger women, and tend to be found in women over the age of 60. Overall, vascular calcifications may appear on about 9% of all mammograms, but for women over 65, about 50% will have developed vascular calcifications. Vascular calcifications have a typical appearance on mammogram (see below) are innocent and do not cause any diagnostic confusion.
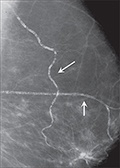
Calcifications are usually too small to be felt. They can be seen on a mammogram where they appear as little white spots. Most of the time calcifications are a harmless finding, however, sometimes the area around the calcification can be breast cancer. In these circumstances, the calcifications themselves are not cancerous but the calcification has occurred in disintegrated old cancer cells that were “thrown out in the rubbish” but haven’t yet been disposed of by the body. While they are waiting to be carted away, these old cells disintegrate and calcify.
Types of calcifications
There are two main types of calcifications, macro and micro.
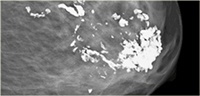
- Macrocalcifications are coarse calcium deposits in the breast. They look like large, white dots or dashes on a mammogram and are often dispersed randomly within the breast (pictured below) Macrocalcifications are common, showing up in about 50 percent of women over 50, and 10 percent of women under 50 years of age. They are a natural result of breast ageing and are harmless. They are not linked with cancer and don’t need any treatment or checking.
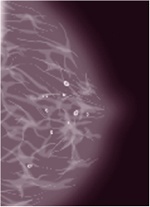
- Microcalcifications are tiny calcium deposits that show up as fine white specks on a mammogram (pictured below) They are usually benign, but can be a warning sign of cancer. 80 percent of microcalcifications are benign.The radiologist looks at the shape and pattern of the microcalcifications to see if they are “suspicious.” More mammograms and a biopsy may be necessary.
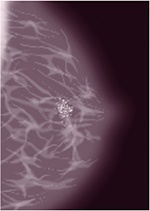
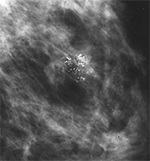
How are calcifications found?
Calcifications are usually found by chance during a routine screening mammogram or while being investigated for another reason. They show up as small white spots.
How are calcifications evaluated?
When you have a mammogram, it’s examined by a radiologist (doctor who specialise in reading x-rays and scans). Calcifications are usually evaluated with X-ray magnification views. With these magnified X-rays, the radiologist can better tell the size, shape and number of calcifications.
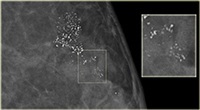
Using this information, the radiologist categorizes the calcifications as:
- Benign
- Indeterminate- probably benign
- Suspicious
If your calcifications look benign, then nothing more needs to be done. If your calcifications look indeterminate or suspicious you will need further tests.
Benign calcifications are of no medical concern and will be evaluated on future mammograms by comparing images from year to year.
Probably benign calcifications are around 98% likely to be benign.
Suspicious calcifications may be seen in either benign or malignant (cancerous) situations.
The benign ones can be left alone, they don’t need to be removed and won’t cause you any harm. The suspicious ones need to be biopsied, and the indeterminate or “can’t tell” ones can either be followed up at an interval (usually 6-12 months) or biopsied. If the radiologist isn’t sure but thinks microcalcification is benign, they will often ask patients to come back in six months for another mammogram.
If, on the other hand, they have any worries, they will recommend a biopsy. Overall only about one of every four women with calcifications thought to be concerning enough to warrant biopsy has a breast cancer, usually at an early preinvasive stage (DCIS).
Because calcifications are so small, a computer and mammogram are usually required to locate and target them accurately, so that a needle biopsy can be taken – this is called a stereotactic biopsy.
Hookwire Localisation
Your doctors may sometimes recommend surgery to remove the area of the calcification from the breast. This is usually only done when a needle core biopsy has been unsuccessful at removing enough of the calcification, or when the result is not definite. In this case a technique called preoperative hookwire localisation is used to pinpoint the area for the surgeon as it can’t be felt.
There are two parts to preoperative hookwire localised breast surgery:
- inserting a hookwire under local anaesthetic before the operation; and
- removing the calcification under general anaesthetic during an operation.
Before the operation –inserting the hookwire
The hookwire will be inserted by a radiologist. Before the operation, you will go to the breast department. The abnormal area in the breast will be identified with a mammogram. An injection of local anaesthetic will be given to numb part of the breast and the hookwire will be inserted under the guidance of the mammogram. A mammogram will also be performed after the wire has been inserted. This mammogram is performed with minimal pressure on the breast so that it does not make the wire move. This checks the position of the wire and helps the surgeon plan the operation. Once the wire is in position, it will be taped in place and a dressing will be applied.
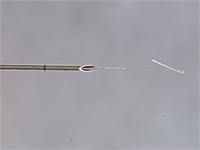 Hookwire inside insertion needle
Hookwire inside insertion needle
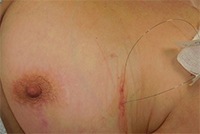 Hookwire in place post insertion
Hookwire in place post insertion
The operation – removing the calcification
Once the hookwire is in position you will be taken to the operating theatre. The operation will be performed under general anaesthetic. The surgeon will remove the piece of tissue at the tip of the wire. Once the tissue is removed, it will be returned to the imaging department where an X-ray of the tissue will be performed to confirm that the calcification is in the tissue that has been successfully removed. The specimen will then be sent to the pathologist.
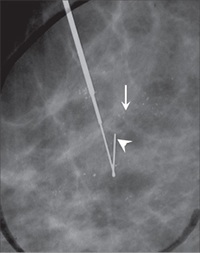 Post hookwire insertion
Post hookwire insertion
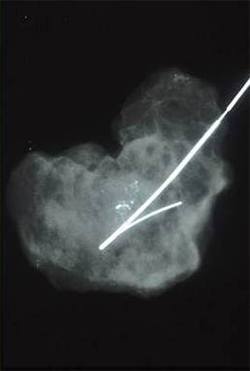 Specimen X-ray showing calcifications
Specimen X-ray showing calcifications
You will need the Adobe Reader to view and print these documents.![]()
Error: Contact form not found.











