Body Weight and Breast Cancer
Being overweight or obese is a risk factor for breast cancer among postmenopausal women, and as such, a disproportionate number of women with breast cancer are above their ideal body weight at the time of diagnosis. It is known that overweight and obese survivors of breast cancer experience poorer outcomes, yet a 2016 study demonstrated that approximately half of overweight and obese breast cancer survivors reported no weight-related discussion with a member of their health care team. The oncology team—the health professionals with whom a patient has the closest relationships in the critical period after a breast cancer diagnosis—is in a unique position to help patients lose weight and make other healthy lifestyle changes.
Cancer clinicians need to address obesity openly with their patients from the time of diagnosis and during follow-up visits. Research shows that the time after a cancer diagnosis can serve as a “teachable moment” to motivate individuals to adopt risk-reducing behaviours. Cancer clinicians should routinely talking to breast cancer patients and survivors about their body mass index/weight status, and the role of healthy eating and exercise on reducing fatigue, improving body image, and lowering incidence of comorbidity.
Patients supply height and weight details on their patient registration form, and this is used to calculate BMI.
Excess body weight is a significant risk factor for many cancers, especially breast cancer. Patients with breast cancer or those with a history of the disease who are overweight or obese have an increased risk of therapy-related morbidity, recurrence, and breast cancer–related mortality. Obesity may also affect quality-of-life factors for survivors, including sexual dysfunction, neuropathy, cardiotoxicity, chronic fatigue, and lymphoedema. Most cancer guidelines recommend that breast cancer survivors who are overweight or obese lose weight and that those with a normal body mass index (BMI) maintain a stable body weight. The cornerstone of interventions to treat or prevent obesity is lifestyle modification with diet and exercise; however, integrating these into clinical practice is challenging.



- Obese postmenopausal women are at increased risk of developing hormone receptor positive breast cancer.
- Obesity at the time of breast cancer diagnosis is a poor prognostic factor in both premenopausal and postmenopausal women, with a higher risk of recurrence and mortality.
- Obesity is a risk factor for poor wound healing and postoperative infection.
- Obesity places individuals at an increased risk of developing second primary malignancies.
- Obesity can interfere with the effective delivery of systemic breast cancer therapy and can contribute to morbidity from treatment.
- Obesity is a risk factor for the development of comorbid illness (eg, heart disease, cerebrovascular disease and diabetes), in breast cancer survivors.
- Obesity may affect quality-of-life factors for survivors, including sexual dysfunction, neuropathy, cardiotoxicity, chronic fatigue, and lymphoedema.
Weight and Breast Cancer Risk.
Most reports have suggested that obesity is associated with an increase in hormone receptor–positive postmenopausal breast cancer, but not in hormone receptor–negative disease. A secondary analysis of the Women’s Health Initiative demonstrated a 52% increase in the risk of hormone receptor–positive breast cancer in obese vs normal-weight women but no significant increase in the risk of hormone receptor–negative cancers. There is an estimated12% increase in the risk of developing breast cancer for each 5-point increase in body mass index (BMI).
Studies have shown that obese premenopausal women are at slightly lower risk of developing breast cancer compared with their normal-weight counterparts.
It is not well understood why obesity is associated with an increased risk of postmenopausal hormone receptor–positive breast cancer but a decrease in the risk of premenopausal hormone receptor–positive breast cancer. One hypothesis for the pathophysiology relating obesity to breast cancer risk focuses on the differential impact of obesity on sex hormone levels in premenopausal and postmenopausal women. Postmenopausal women derive oestradiol from peripheral conversion of androgens by the enzyme aromatase. Adipose tissue is rich in aromatase, which results in obese women having higher levels of oestradiol. Overall, approximately 15% of breast cancer cases in postmenopausal women may be attributable to elevated weight.
Weight and Breast Cancer Mortality
Weight at Diagnosis
Obese patients with breast cancer have an increased relative risk of recurrence of 40% to 50% and a relative risk of breast cancer–related mortality of 53% to 60%. Obese women with hormone receptor–positive operable breast cancer have inferior outcomes in terms of disease-free survival and overall survival compared with non-obese women.
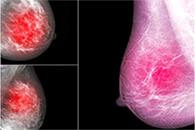

Obese women with breast cancer have worse overall survival and breast cancer–specific survival than nonobese women. Several recent meta-analyses have demonstrated an association between being overweight or obese at the time of breast cancer diagnosis and increased risk of breast cancer–specific and all-cause mortality. A 2014 meta-analysis that included 82 individual studies encompassing 213,075 women and 41,477 deaths found a 41% increased risk of total mortality and a 35% risk of breast cancer–specific mortality for obese women compared with normal-weight women. For each 5-point increase in BMI, there was an 18% increase in the risk of breast cancer mortality and an association between mortality and BMI at the time of diagnosis, less than 1 year after diagnosis, and greater than 1 year after diagnosis, demonstrating a persistent relationship between obesity and poor outcomes over time.
The relationship between BMI and breast cancer mortality is seen in both premenopausal and postmenopausal women, with obese premenopausal women having a 75% higher chance of overall mortality and obese postmenopausal women having a 34% higher chance of overall mortality.
Weight Change After Diagnosis
Weight gain during or after breast cancer treatment increases the risk of recurrence and reduces survival, irrespective of baseline body mass index. Women who gain weight during or after treatment of breast cancer have been consistently shown to be at higher risk of breast cancer–related death.
Most patients with breast cancer gain weight both during and after active treatment, and much of the weight is never lost. The average reported weight gain is 2.5–5 kg, but a gain of 10 kg or more is not uncommon. The reasons for weight gain are multifactorial and include “stress eating,” reduced activity because of fatigue or other treatment-related adverse effects, lowered metabolic rate from chemotherapy, and use of pre- and post-chemotherapy medications such as dexamethasone. Weight gain is most common in women who experience treatment-related menopause and is often accompanied by relative fat gain and muscle loss.



From 1997 to 2014, obesity increased more rapidly among adult cancer survivors compared with the general population, with the prevalence of obesity increasing from 22.4% to 31.7% in cancer survivors and from 20.9% to 29.5% in adults without a history of cancer. The estimated rate of annual increase in obesity prevalence was 3.0% in breast cancer survivors.
Several observational studies have shown that gaining weight during or after breast cancer treatment increases the risk of recurrence and reduces survival, irrespective of baseline body mass index (BMI). In a recent meta-analysis of 12 studies on weight gain after diagnosis, weight gain of more than 10% was associated with increased mortality.
Weight and Other Adverse Outcomes in Women With Breast Cancer
Second Primary Malignancies
Obesity increases the risk that survivors of breast cancer will develop a second primary malignancy. A recent meta-analysis found that obesity was associated with a 37% increase in the relative risk (RR) of contralateral breast cancer, a 97% increase in the RR of endometrial cancer and an 89% increase in the RR of colorectal cancer in breast cancer survivors. These findings are likely to be related to the fact that obesity is a risk factor for developing breast, endometrial, and colorectal primary cancers in the general population.
Lymphoedema
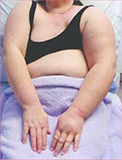
Lymphoedema of the arm is a known complication of breast cancer treatment. Greater extent of local therapy and obesity are the two most important and significant risk factors for developing this condition. At least 14 studies have found an association between obesity and lymphoedema. Cancer treatments such as lymph node dissection and radiation therapy can damage lymphatic drainage routes, leading to fluid build-up, discomfort, and reduced mobility and function. Excess adiposity may increase risk of lymphoedema via increased inflammation, added stress on the lymphatic system, or slower healing times after surgery. Prospective studies have reported statistically significantly higher lymphoedema risk for obese compared with normal-weight women, and breast cancer survivors who wee obese at the time of treatment were approximately 3.6 times more likely to develop lymphedema at 6 months after diagnosis than those who were not obese. In a pilot study among overweight breast cancer survivors, a 12-week diet intervention resulted in a significant reduction in BMI and swollen arm volume (reduced from 24% to 15%).
Neuropathy
Chemotherapy-induced peripheral neuropathy (CIPN) has been reported in up to 44% of patients receiving chemotherapy, particularly taxanes, and is more common in obese patients, Higher BMI is associated with a higher incidence of neuropathy, with studies demonstrating a prevalence of 48.4% in participants with normal weight, 60.2% in overweight participants, and 66.7% in obese participants. Neuropathy was significantly more likely to occur in overweight patients compared with normal-weight patients receiving taxane treatment at 24 months, and less likely to occur in patients with high moderate-to-vigorous physical activity levels compared with those with lower activity levels at 24 months. While studies have not shown that weight loss can reverse neuropathy, these data suggest that physical activity may help.
Cardiotoxicity
Because obesity is already a strong risk factor for cardiovascular disease, cancer treatment in obese patients can further increase overall risk for adverse cardiac effects. A recent meta-analysis suggests that being overweight or obese may be a risk factor for cardiotoxicity from anthracyclines, especially when these are administered in sequence with trastuzumab (Herceptin). Other studies have found obesity to be associated with an increased risk of cardiac dysfunction in women using trastuzumab. Additionally, in elderly patients (over 65 years of age), obesity is an independent risk factor for trastuzumab-related cardiac toxicity.
Chronic fatigue
About one-third of breast cancer survivors have chronic fatigue and about one-fourth will have persistent fatigue after 2 years. Although the development of fatigue in breast cancer patients seems largely due to cancer therapy, the long-term persistence of fatigue is related to preexisting medical conditions and lifestyle factors. Higher BMI at baseline is significantly associated with increased physical fatigue during and after cancer treatment.
The Mammary Carcinoma Risk Factor Investigation (MARIE) study demonstrated that both a physically inactive lifestyle and obesity were associated with persistent physical fatigue, independent of chemotherapy and radiation therapy. In a study of patients who were overweight or obese, fatigue aft r chemotherapy was lower in an exercise group than in a non-exercise group. Higher BMI, associated with a greater tendency to catastrophize about fatigue and amplify physical symptoms, was predictive of fatigue beyond 9 months. These studies demonstrate the importance of an ideal body weight, since chronic fatigue is associated with emotional distress and limits function and willingness to exercise.
Surgical Complications
Surgical complications are dealt separately. See BODY WEIGHT AND BREAST SURGERY COMPLICATIONS
References:
- Obese Breast Cancer Patients and Survivors: Management Considerations, Sheng et al, The Oncology Journal, 2018.
- Obesity and Breast Cancer: Risk, Outcomes, and Future Considerations, Ligibel et al, Clinical Advances in Hematology & Oncology, 2016.
- Lifestyle modifications for patients with breast cancer to improve prognosis and optimize overall health, Warner et al, CMAJ, 2017.
Common Challenges to Losing and Maintaining Weight
Before being diagnosed with breast cancer, you may have already tried to lose weight or increase physical activity and found the results discouraging. The section below addresses common beliefs that may prevent people with cancer from pursuing a healthier lifestyle.
“I’VE TRIED EVERYTHING AND JUST CAN’T LOSE WEIGHT.”
Losing weight is challenging. You may feel you have “failed” because previous attempts to lose weight have not worked. You haven’t failed; you just haven’t found what works for you yet. Talking with your doctor or asking for a referral to a registered dietitian or a weight-loss group can help find the best method for you. Many people find it easier to lose weight if they have a structured programme and support.
“I DON’T REALLY WANT TO EXERCISE.”
Starting an exercise program may seem overwhelming, and cancer treatments can make you tired or cause changes in your mobility. However, participating in physical activity can actually improve your energy level. There are ways to make starting easier. First, pick an activity you enjoy. You’re more likely to stick with activities you look forward to. It’s important to remember that physical activity comes in many forms, such as walking, dancing, playing actively with your children or grandchildren, or gardening. Second, start small. If you have been very inactive, start with just 10 minutes a day and increase the time gradually.
“I ENJOY EATING AND DON’T WANT TO CHANGE MY DIET.”
You can still enjoy the foods you love, but with more balance. For most people, there is no need to participate in an extremely restrictive diet plan. The goal is to eat fewer calories. Even small reductions or changes to what you eat and drink can help you lose weight slowly over time. Working with a dietitian can help you lose weight while eating the foods you enjoy.
“I’M ALREADY STRESSED ABOUT DEALING WITH MY CANCER.”
Cancer is definitely stressful, partially because there are so many factors that are out of your control. Fortunately, physical activity lowers stress and improves the symptoms of anxiety and depression for many people. In addition, focusing on losing weight and exercising can add some feeling of control to your life.
“THE HARM HAS ALREADY BEEN DONE.”
It is never too late to improve your health. Many studies have shown that people who choose healthy foods and exercise regularly are at lower risk of having the cancer return or of developing a new cancer. In addition, changing to a healthier lifestyle reduces the risk of other medical problems, such as diabetes and heart disease, which may be more of a threat to your overall health than cancer.
The St Vincent’s Private East Melbourne Oncology Rehabilitation Programme
We encourage all our breast cancer patients to participate in The St Vincent’s Private East Melbourne Oncology Rehabilitation Programme.This 6-week outpatient program aims to facilitate recovery from cancer allowing the individual to return to an active and satisfying life. The oncology rehabilitation program comprises an organised group program that combines health education, exercise and support. We provide each patient with an individual, supervised exercise program and specific referrals to members of the multi-disciplinary team, where appropriate. The programme can be undertaken either prior to breast cancer surgery, in patients undergoing preoperative (neoadjuvant) chemotherapy or after surgery.
The program includes:
- An initial assessment by a physiotherapist and rehabilitation physician.
- A customized exercise program supervised by an oncology physiotherapist.
- A comprehensive education program focused on support after cancer, management of treatment related side-effects and encouraging a healthy lifestyle to prevent cancer recurrence.
- Expert physiotherapist advice on managing treatment related impairments.
- Access to an open forum for both patients and support members to ask questions and share experiences.



Our Staff
Our multi-disciplinary team includes a:
- rehabilitation physician.
- oncology liaison nurse.
- oncology physiotherapist.
- occupational therapist.
- dietitian.
- psychologist.
- The cost of this program is covered by most private health insurance funds. We will complete a health fund check and notify you of any cost involved prior to commencement of the program.
- Parking is available at no cost to all patients attending the program.
- Managing Your Weight After a Cancer Diagnosis- A Guide for Patients and Families
- Healthy Eating and Breast Cancer
- Diet and breast cancer
- Obesity and Nutrition and Lifestyle After Breast Cancer
- Nutrition and Cancer – A guide for people with cancer, their families and friends
- A Nutrition Guide for Women with Breast Cancer
- Oncology Day Therapy Rehabilitation at St Vincent’s Private Hospital East Melbourne
Costs
Program details
When : Every Monday and Wednesday for 6 weeks, from 1.00 pm – 3.00 pm or 2 pm – 4 pm (Group sessions)
Where : Ground floor, 166 Gipps St East Melbourne, 3002.
Patient Information on Diet and Breast Cancer
You will need the Adobe Reader to view and print these documents.![]()
Error: Contact form not found.











