Smoking and Breast Surgery Complications
Smoking and Breast Surgery Complications
Smoking can increase the complication rate of breast surgery by up to 40-60%. Smoking increases the risk of anaesthetic, medical and surgical complications associated with breast surgery.
Nicotine can affect cardiovascular health in many ways. It increases blood pressure and constricts (shrinks) blood vessels. The nicotine in just one cigarette stimulates the smooth muscle fibres in the wall of the blood vessels to contract, which shrinks the blood vessels and makes them narrower. Narrower blood vessels cannot carry as much blood to the tissues. Less blood flow means less oxygen, essential nutrients and growth factors are delivered to the tissues. This increases the risk of complications like poor wound healing, infection, blood clots, and even loss of some or all of the reconstruction.
Complications that may arise due to mixing smoking with breast surgery include:
- Wound Infections.
- Tissue death (necrosis)
- Prolonged healing time
- Implant loss
- Scars that are more visible than usual
- Problems with anaesthesia or the need for a ventilator after surgery
- Increase in the likelihood of life-threatening complications (such as stroke, heart attack and pneumonia)
- Post-operative chest infections or persistent coughs
- Increased pain
- Blood clots
Smoking is a significant and independent risk factor for the development of wound complications following surgery for breast cancer. Other risk factors are obesity, diabetes and previous radiation.




Patients with a history of smoking have a 6.5 times greater risk of developing complications following breast surgery. In patients undergoing mastectomy, the increased risk of developing skin flap necrosis for heavy and light smokers is 9.22 and 6.85 times respectively. (2)
General anaesthesia complications: During breast surgery, your anaesthetist will put you to deep sleep (general anaesthesia). Smoking is well-known to damage your lungs, and it does this by destroying the fine hair-like cilia on your lung cells that are responsible for clearing your airways from mucus and debris. This puts you at higher risk of developing pneumonia (lung infection) or collapsed lungs after surgery. Carbon monoxide in the body from smoking also lowers blood oxygen levels, making it more difficult for your heart and lungs to work while under anaesthesia.
You are more likely to have a painful recovery: Nicotine can lower the effectiveness of certain pain medications or interfere with the way they work, impacting healing and leading to greater discomfort after surgery.
Smoking increases risk of blood clots: The chemicals in cigarettes thicken the blood. Thick, sticky blood likes to clot. If a clot forms and travels to the heart or lungs, a life-threatening pulmonary embolism can occur.
Smokers are 38% more likely to die after surgery than non-smokers. Following surgery, smokers:
- have higher risks of post-operative infection
- have impaired wound healing
- require longer hospital stays and higher drug doses
- have increased risk of emergency re-admission
- are more likely to be admitted to an intensive care unit
- have increased risk of emergency re-admission
- have higher risks of lung and heart complications

How does smoking affect wound healing after breast surgery?
Numerous studies have shown that smoking delays wound healing, increases the risk of wound infection, skin sloughing (necrosis), and interferes with how your scar will look. Several mechanisms explain how smoking can cause wound complications in patients undergoing surgery:
- Smoking reduces oxygen supply to the wound: Oxygen is essential to proper wound healing, and smoking prevents enough oxygen from reaching your tissue, a condition known as hypoxia or ischemia. Carbon monoxide, one of the known toxins in cigarette smoke, binds to haemoglobin, the oxygen transporter in your blood. This prevents haemoglobin from carrying oxygen to the tissue and deprives your cells of their supply. The nicotine in tobacco smoke causes your blood vessels to shrink and become narrow, so less blood will reach your skin and wound. Moreover, nicotine increases your heart rate and your blood pressure, which can stress your heart and even damage it, causing further oxygen deprivation in your body.
- Smoking impairs cell functions: Several types of cells are involved in the wound healing process, and they usually determine how quickly your wound will heal, and how your scar will look after healing. Cigarette smoke also inhibits the normal function of fibroblasts and myofibroblasts, cells imperative to normal wound healing Cigarette smoke inhibits the normal migration patterns of fibroblasts, and fibroblasts remain at the wound edge and fail to migrate to the centre of the wound, causing excessive scar at wound edges without proper collagen formation in the wound. This means that if you smoke, while your wound may be weak, the scar may end up more obvious.
- Smoking impairs immunity: Smoking cigarettes weakens your immunity and makes you more prone to developing infections. If you’re having surgery, you will be more likely to develop a wound infection, which can dramatically affect how your wound will heal, and how it will eventually look.
- Smoking increases the risk of blood clots: The nicotine in tobacco smoke stimulates the release of certain chemicals in the body that make your blood more sticky and thick. This increases the risk of developing small blood clots that obstruct your blood vessels and deprive your wound of blood and oxygen supply.
Some of the wound complications that can occur, often found in combination, include:
- Wound infection/cellulitis: Smokers have weakened immunity, so if any infective complication occurs, might not be able to fight off the offending microbes. Staphylococcal organisms coming from the skin flora are usually implicated in postoperative wound infections following breast surgery
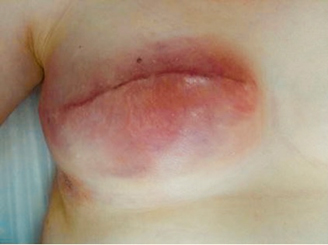
Smokers are also more likely to develop cellulitis, which is a type of bacterial skin infection that can occur anywhere in the body, that affects skin tissues just underneath the skin’s surface. Staphylococcus aureus and Streptococcus are the two most common types of bacteria that cause cellulitis. A decreased immune system can increase your risk for cellulitis, and breast cellulitis mostly manifests itself from cancer treatments or surgeries.
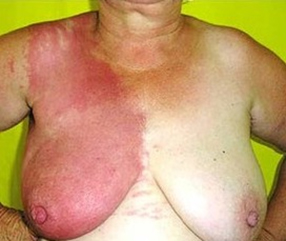
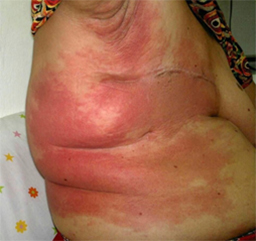
Cellulitis
- Delayed wound healing: In smokers, surgical wounds take longer to heal, which increases the risk of developing even more complications. Delayed healing of a surgical incision is not uncommon in breast surgery. Its severity can vary from simple delay of the healing process to actual failure of the suture line and true dehiscence. Tissue necrosis is not a prerequisite; loss of the ability of tissues to heal in a timely manner is enough to cause this complication.
- Wound dehiscence: You have 4 to 6 weeks to heal internally before the dissolvable stitches start to dissolve. If you haven’t healed adequately by then, you may open up. Dehiscence might sometimes require a vacuum dressing or a re-operation to repair.
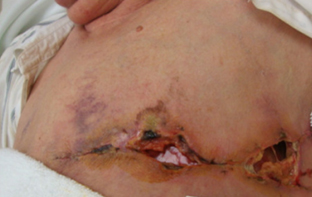
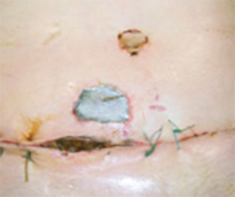
Mastectomy wound dehiscence Dehiscence of lower abdominal flap donor site
- Skin/tissue necrosis: When your skin cells don’t receive enough blood and oxygen, they’re likely to die and slough off. This is much more likely to happen if you’re a smoker.
The wound problems above often occur in combination. For example, the skin edge blood supply being poor because of smoking, may lead to an are of necrotic (dead) skin, which fails to heal, the wound parts and allows the ingress of normally harmless skin flora (staph).
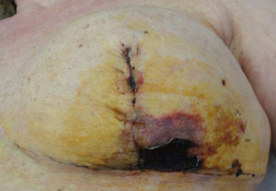
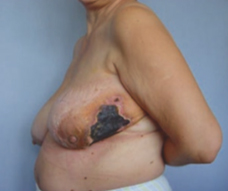
Skin Necrosis
- Unpleasant/prominent scarring: Smoking increases scarring, and makes scars larger and more noticeable.
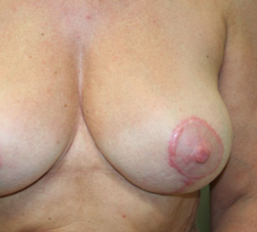
Smoking and Breast Reconstruction Complications
Smoking can particularly cause serious complications for breast reconstruction
Smoking is well known to cause major issues with wound healing after breast reconstruction. Current smokers are more likely to have mastectomy flap loss, wound separation, and skin/tissue loss (necrosis) than non-smokers. In a 2001 study almost 40% of the smokers undergoing breast reconstruction experienced complications, such as mastectomy flap necrosis, fat necrosis, abdominal wall necrosis, seroma, wound dehiscence, and infection, compared with about 25% of non-smokers and ex-smokers. (4)
For women who have implants placed, smokers are more likely to need their prostheses removed due to complications (such as infection) when compared to those who do not smoke. Those who smoke while on chemotherapy for their breast cancer also are more likely to need the prostheses removed than those who are on chemotherapy for their breast cancer but do not smoke. Wound infections are never trivial, but in certain clinical situations they can have particular, deleterious sequelae. Immediate breast reconstruction may be desirable for some patients after mastectomy. An infected prosthesis, or necrosis of a flap or tissue donor site, can delay important adjuvant chemotherapy or radiotherapy.
Regarding breast reconstruction, two studies showed higher rates of reconstructive failure and overall complications in smokers. However, no significant difference was found regarding flap loss and vascular thrombosis between smokers and non-smokers.

Advice from a health professional is the second most common reason patients give for stopping smoking, and the more times patients hear the message, the more likely they are to act on it. Patients awaiting surgery can play an active role in achieving good outcomes, and stopping smoking is one of the most important measures that they can take. Surgeons need to ensure that patients understand the harms of continuing to smoke before surgery, and the benefits of quitting.
Although patients may initially resist the intervention on the grounds that a cigarette will help them get through the stress of surgery, it is vital that health professionals help them understand why stopping smoking is so important. It is sometimes difficult to effectively communicate to a smoking patient that their smoking habit places them at an unacceptable level of risk for preventable surgical complications. To many patients, complications following a surgical procedure are not very tangible. Patients seem to place great faith in the wonders of modern medicine to shield them from surgical morbidity and mortality.
Often there is minimal patient insight that activities such as smoking could produce devastating complications. Most patients are intolerant of complications and may tend to project blame towards the operating surgeon versus accepting that their smoking has contributed in any meaningful manner. It is important to have a frank discussion regarding the issue of smoking with patients. Patients may take this matter more seriously if you can portray to them the nature of infection, delayed wound healing or skin necrosis in terms of hospital readmissions, revisionary surgery, wound debridement and scarring.
In the context of purely elective surgery, it is easier to avoid a devastating complication by refusing to operate on actively smoking patients due to unacceptable risk or require a designated period of complete abstinence from smoking prior to surgery.
Obviously breast cancer surgery is essential, and needs to be undertaken in a timely manner, however, sometimes it may be deemed that an associated medically non-essential breast reconstruction in a smoker needs to be deferred because the risk of complications is deemed to be too high, and may risk delaying important cancer treatment such as chemotherapy.



How long before breast surgery should you quit smoking?
The optimum period of smoking cessation is uncertain, but it is probably at least 4-6 weeks. If you can’t cease smoking for this long, stopping even as little as 12 hours before your surgery can still have some benefits, albeit rather minimal.
- Quitting smoking for as little as three weeks has been shown to improve wound healing.
- Immune function is significantly recovered by 6 months after quitting smoking.
Reduction rather than cessation in smoking is inadequate. Cutting down on smoking alone without completely quitting will not reduce the rate of complications. You have to give up smoking completely to reverse the damage done by cigarettes on your body’s healing abilities.
Smoking has an immense impact on all phases of wound healing and the microenvironment of the tissue. Specific toxic effects and oxidative stress induced by smoking appear to mediate the principal hazardous mechanisms: ( a temporary reduction in tissue perfusion and oxygenation, impairment of inflammatory cell functions and oxidative bactericidal mechanisms, and attenuation of reparative cell functions including synthesis and deposition of collagen. The attenuation of inflammation and proliferation is ultimately responsible for the higher incidence of healing complications in smokers.
Smoking cessation reverses some of these mechanisms but not all, because many of the pathologic processes induced by smoking appear to be prolonged or even irreversible despite abstinence from smoking. Improvement of inflammatory cell response and bactericidal mechanisms explains the reduction in infectious healing complications after smoking cessation. The persistent impairment of wound proliferation and remodelling after smoking cessation explains why non-infectious healing complications appear to remain more frequent in previous smokers than in never smokers.
We now know that, although earlier is best, stopping smoking even up to the day before surgery can lead to better outcomes. Nowadays, some surgeons will not perform elective surgery until a patient abstains from smoking and, although patients may think they are being penalised for their lifestyle, there is good evidence behind this decision, as the associated risks mean surgery is not always safe when a patient continues to smoke.(8)
How can I quit smoking before surgery?


The role of the surgeon is to identify tobacco users, advise them to quit, and then refer the patients to evidence-based resources that can provide assistance. The point at which the patient and surgeon agree that surgery should take place should be seen as a ‘teachable moment’ where patients are often more receptive to intervention and more motivated to quit. When discussing the risks of any potential procedure the surgeon should outline the reduction in risk associated with smoking cessation. Advice from surgeons to quit smoking is likely to have a big impact on patients and it is important that patients receive consistent messages from all health professionals about smoking.
Quitting smoking is one of the best decisions that anyone can ever take. Smoking cessation is the single most important step you could take to prevent smoking-related illnesses and reduce your risk of heart disease, lung disease, strokes, and cancer. If you’re like all the other smokers that find quitting extremely hard, you’d be glad to know that several methods can help you go through with your decision.
- Quitline: The Australian Department of Health has a dedicated phone line to assist smokers in their journey toward a smoking-free life. Whenever you’re ready, any time of the week, you can call 13 7848 free of charge, and talk to a trained counsellor to get important information, tips, coaching, and support to successfully quit. quit.org.au
- Consider using pharmacotherapy: Different products are available to help you quit smoking. Nicotine replacement therapy (NRT) includes patches, gum, lozenges, inhalers and mouth spray. The aim of NRT products is to replace some of the nicotine from cigarettes without the harmful chemicals found in tobacco smoke, thus reducing withdrawal symptoms, such as cravings and anxiety. You need to know, however, that nicotine-containing drugs can still interfere with normal wound healing.
- Non-nicotinic drug therapy: Bupropion Hcl (Zyban) and Varenicline (Champix) are non-nicotine medications that are also effective in helping smokers to quit. Bupropion Hcl and Varenicline are available only on prescription and your GP can help decide if they are suitable for you.
References:
QUIT Smoking and Surgery DL booklet V5
Smoking as a risk factor for wound healing and infection in breast cancer surgery
Wound Healing and Infection in Surgery
Complications of Postmastectomy Breast Reconstruction in Smokers, Ex-smokers, and Non-smokers
Complications in Smokers After Postmastectomy Implant
Rationing elective surgery for smokers and obese patients- responsibility or prognosis
You will need the Adobe Reader to view and print these documents.
![]()
Error: Contact form not found.











