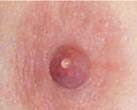
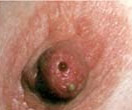
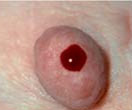
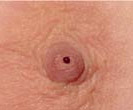
Nipple Discharge
Nipple Discharge – the release of fluid from the nipple – is common, and in most cases benign.
Spontaneous, single duct Nipple Discharge is pathological, and diagnostic surgery will usually be recommended in order to exclude malignancy. The difficulty in managing pathological spontaneous, single duct Nipple Discharge is that the risk of carcinoma, despite being low, cannot be eliminated without surgical duct excision and histologic confirmation. Thus, duct excision in all patients with pathologic single duct Nipple Discharge is widely recommended.
There are 15–20 milk ducts opening onto each nipple. Discharge can come from one or more of these ducts. Nipple Discharge can:
- be spontaneous (fluid is secreted from the nipple without any squeezing of the nipple or pressure on the breast), or
- be on expression (fluid is secreted from the nipple when the nipple is squeezed or there is pressure on the breast)
- originate from one duct (one opening on the nipple) or more than one duct.
- come from one breast (unilateral) or both breasts (bilateral)
- be clear, yellow, milky, brown, green, or bloodstained in appearance
Physiological Nipple Discharge
Discharge of fluid from a normal breast is referred to as ‘physiological discharge’. It is usually yellow, milky, or green in appearance, does not occur spontaneously, and often originates from more than one duct. Physiological Nipple Discharge is no cause for concern. Milky Nipple Discharge is also normal during pregnancy and breastfeeding.
When is Nipple Discharge abnormal?
Spontaneous Nipple Discharge unrelated to pregnancy or breastfeeding is considered abnormal. In most cases it has a benign cause, and is more likely to be unilateral, confined to one duct, and clear or bloodstained in appearance. Nipple Discharge associated with other breast symptoms such as a lump, ulceration, or inversion of the nipple require prompt investigation.
What are the causes of abnormal Nipple Discharge?
- Duct ectasia This is a benign condition in which there is enlargement of the milk ducts under the nipple with inflammation in the walls of the ducts. It usually occurs in women after menopause. The discharge is usually bilateral, yellow, clear, or green in appearance and arises from multiple ducts. In most cases, no treatment is required
- Duct papilloma This is a growth within a milk duct in the breast, usually near the nipple. It may cause no symptoms, or a discharge that is clear or bloodstained. Duct papillomas are almost always benign. On occasions, they may be associated with breast cancer. Because of this association, they are usually surgically removed.
- Breast cancer Breast cancer is an uncommon cause of Nipple Discharge. Few women with breast cancer have Nipple Discharge, and most have other symptoms, eg. a lump or newly inverted nipple.
- Hormonal causes Galactorrhoea is a milky Nipple Discharge unrelated to pregnancy or lactation. It is caused by the abnormal production of a hormone called prolactin which is caused by diseases of glands elsewhere in the body that control hormone secretion, eg. pituitary and thyroid glands
- Drugs and medications Some drugs can cause abnormally high prolactin levels including oral contraceptives, hormone therapy, and medications used for the treatment of nausea, depression and psychiatric disorders. Drugs such as cocaine and stimulants can also cause high prolactin levels.
How is Nipple Discharge investigated and treated?
About 5% of breast referrals are with this symptom, and of these only about 5% will prove to have cancer.
Physiological Nipple Discharge requires no treatment. It is important to stop expressing or squeezing the nipple and breast as this causes more fluid to be produced. The discharge will usually stop when you stop expressing.
Spontaneous, persistent Nipple Discharge unrelated to pregnancy or breastfeeding needs investigation by examination and imaging of the breast. Nipple Discharge loses its significance when it is accompanied by a lump. The lump then takes precedence in assessment and management.
Spontaneous, single duct Nipple Discharge is pathological, and diagnostic surgery is widely recommended in order to exclude malignancy.
Error: Contact form not found.